What are migraines?
Migraines are a recurring type of headache. They cause moderate to severe pain that is throbbing or pulsing. The pain is often on one side of your head. You may also have other symptoms, such as nausea and weakness. You may be sensitive to light and sound.
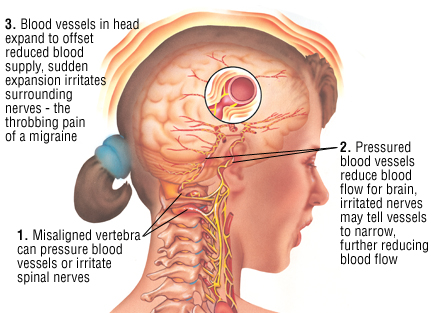
What causes migraines?
Researchers believe that migraine has a genetic cause. There are also a number of factors that can trigger a migraine. These factors vary from person to person, and they include
- Stress
- Anxiety
- Hormonal changes in women
- Bright or flashing lights
- Loud noises
- Strong smells
- Medicines
- Too much or not enough sleep
- Sudden changes in weather or environment
- Overexertion (too much physical activity)
- Tobacco
- Caffeine or caffeine withdrawal
- Skipped meals
- Medication overuse (taking medicine for migraines too often)
Some people have found that certain foods or ingredients can trigger headaches, especially when they are combined with other triggers. These foods and ingredients include
- Alcohol
- Chocolate
- Aged cheeses
- Monosodium glutamate (MSG)
- Some fruits and nuts
- Fermented or pickled goods
- Yeast
- Cured or processed meats
Who is at risk for migraines?
About 12% of Americans get migraines. They can affect anyone, but you are more likely to have them if you
- Are a woman. Women are three times more likely than men to get migraines.
- Have a family history of migraines. Most people with migraines have family members who have migraines.
- Have other medical conditions, such as depression, anxiety, bipolar disorder, sleep disorders, and epilepsy.
What are the symptoms of migraines?
There are four different phases of migraines. You may not always go through every phase each time you have a migraine.
- Prodome. This phase starts up to 24 hours before you get the migraine. You have early signs and symptoms, such as food cravings, unexplained mood changes, uncontrollable yawning, fluid retention, and increased urination.
- Aura. If you have this phase, you might see flashing or bright lights or zig-zag lines. You may have muscle weakness or feel like you are being touched or grabbed. An aura can happen just before or during a migraine.
- Headache. A migraine usually starts gradually and then becomes more severe. It typically causes throbbing or pulsing pain, which is often on one side of your head. But sometimes you can have a migraine without a headache. Other migraine symptoms may include
- Increased sensitivity to light, noise, and odors
- Nausea and vomiting
- Worsened pain when you move, cough, or sneeze
- Postdrome (following the headache). You may feel exhausted, weak, and confused after a migraine. This can last up to a day.
Migraines are more common in the morning; people often wake up with them. Some people have migraines at predictable times, such as before menstruation or on weekends following a stressful week of work.
What is the Triggers of Migraine ?
Some common migraine triggers include:
- Hormone changes. Many women notice that they have headaches around their period, while they’re pregnant, or when they’re ovulating. Symptoms may also be tied to menopause, birth control that uses hormones, or hormone replacement therapy.
- Stress. When you’re stressed, your brain releases chemicals that can cause blood vessel changes that might lead to a migraine.
- Foods. Some foods and drinks, such as aged cheese, alcohol, and food additives like nitrates (in pepperoni, hot dogs, and lunchmeats) and monosodium glutamate (MSG), may be responsible in some people.
- Skipping meals
- Caffeine. Getting too much or not getting as much as you’re used to can cause headaches. Caffeine itself can be a treatment for acute migraine attacks.
- Changes in weather. Storm fronts, changes in barometric pressure, strong winds, or changes in altitude can all trigger a migraine.
- Senses. Loud noises, bright lights, and strong smells can set off a migraine.
- Medications. Vasodilators, which widen your blood vessels, can trigger them.
- Physical activity. This includes exercise and sex.
- Tobacco
- Changes to your sleep. You might get headaches when you sleep too much or not enough.
What is Migraine Types ?
Migraine can be classified into subtypes, according to the headache classification committee of the International Headache Society:
-
Migraine without aura is a recurrent headache attack of 4 to 72 hours; typically unilateral in location, pulsating in quality, moderate to severe in intensity, aggravated by physical activity, and associated with nausea and light and sound sensitivity (photophobia and phonophobia).
-
Migraine with aura has recurrent fully reversible attacks, lasting minutes, typically one or more of these unilateral symptoms: visual, sensory, speech and language, motor, brainstem, and retinal, usually followed by headache and migraine symptoms.
-
Chronic migraine is a headache that occurs on 15 or more days in a month for more than three months and has migraine features on at least eight or more days in a month.
-
Complications of migraine
-
Status migrainosus is a debilitating migraine attack that lasts more than 72 hours.
-
Persistent aura without infarction is an aura that persists for more than one week without evidence of infarction on neuroimaging.
-
Migrainous infarction is one or more aura symptoms associated with brain ischemia on neuroimaging during a typical migraine attack.
-
Migraine aura-triggered seizure occurs during an attack of migraine with aura, and a seizure is triggered.
-
-
Probable migraine is a symptomatic migraine attack that lacks one of the features required to fulfill criteria for one of the above and does not meet the criteria for another type of headache.
Episodic syndromes that may be associated with migraine
-
Recurrent gastrointestinal disturbances are recurrent attacks of abdominal pain and discomfort, nausea, and vomiting that may be associated with migraines.
-
Benign paroxysmal vertigo has brief recurrent attacks of vertigo.
-
Benign paroxysmal torticollis is recurrent episodes of head tilt to one side.
How are migraines diagnosed?
For migraines without aura, diagnostic criteria include:
-
5+ attacks fulfilling the other criteria
-
Headache attacks that last from 4 to 72 hours (untreated or unsuccessfully treated)
-
Headache consisting of at least 2 of the following characteristics: unilateral location, pulsating quality, moderate/severe pain intensity, and aggravation by or causing avoidance of routine physical activity (i.e., walking or climbing stairs)
-
During the headache, the presence of at least one of the following: nausea/vomiting, photophobia/phonophobia
-
Not better accounted for with another ICHD-3 diagnosis
For migraines with aura, diagnostic criteria include:
-
Two or more attacks fulfilling the other criteria
-
At least one of the following completely reversible symptoms of aura: visual, sensory, motor, speech or language, brainstem, retinal
-
At a minimum of three of the following six characteristics: 1+ one aura symptoms spread gradually over greater than equal to 5 minutes, 2+ aura symptoms occur in succession, each aura symptom lasts 5-60 minutes, 1+ aura symptom is unilateral, 1+ aura symptom is positive, the aura is accompanied or followed within 60 minutes by the headache
-
Not better accounted for with another ICHD-3 diagnosis
For chronic migraine, diagnostic criteria include:
-
Headache (migraine-like or tension-type-like) on greater than or equal to 15 days/month for greater than three months and also fulfilling criteria B and C
-
Occurring in a patient who has experienced at least five attacks fulfilling criteria B through D for migraine presenting without aura and/or criteria B and C for migraine that presents with aura
-
Occurs greater than or equal to 8 days/month for greater than three months, fulfilling any of the following
-
Criteria C and D for migraine without aura
-
Criteria B and C for migraine with aura
-
Believed by the patient to be migraine at the point of onset and relieved by a triptan or ergot derivative
-
Not better accounted for with another ICHD-3 diagnosis
How are migraines treated?
There is no cure for migraines. Treatment focuses on relieving symptoms and preventing additional attacks.
There are different types of medicines to relieve symptoms. They include triptan drugs, ergotamine drugs, and pain relievers. The sooner you take the medicine, the more effective it is.
There are also other things you can do to feel better:
- Resting with your eyes closed in a quiet, darkened room
- Placing a cool cloth or ice pack on your forehead
- Drinking fluids
There are some lifestyle changes you can make to prevent migraines:
- Stress management strategies, such as exercise, relaxation techniques, and biofeedback, may reduce the number and severity of migraines. Biofeedback uses electronic devices to teach you to control certain body functions, such as your heartbeat, blood pressure, and muscle tension.
- Make a log of what seems to trigger your migraines. You can learn what you need to avoid, such as certain foods and medicines. It also help you figure out what you should do, such as establishing a consistent sleep schedule and eating regular meals.
- Hormone therapy may help some women whose migraines seem to be linked to their menstrual cycle
- If you have obesity, losing weight may also be helpful
If you have frequent or severe migraines, you may need to take medicines to prevent further attacks. Talk with your health care provider about which drug would be right for you.
Certain natural treatments, such as riboflavin (vitamin B2) and coenzyme Q10, may help prevent migraines. If your magnesium level is low, you can try taking magnesium. There is also an herb, butterbur, which some people take to prevent migraines. But butterbur may not be safe for long-term use. Always check with your health care provider before taking any supplements.
What is the Medicines for Migraine ?
1) Abortive Treatments
1.Anti-inflammatories (NSAIDs and Acetaminophen)
Non-steroidal anti-inflammatory drugs (NSAIDs) are mainstay choices and have the greatest strength of evidence. Ibuprofen, naproxen sodium, acetylsalicylic acid (ASA), and diclofenac potassium all have double-blinded randomized controlled trial evidence for efficacy that has analysis in systematic reviews.
NSAIDs include aspirin, naproxen, ibuprofen, tolfenamic acid, diclofenac, piroxicam, ketoprofen, and ketorolac.
Acetaminophen and the combination of acetaminophen/aspirin/caffeine have also demonstrated consistent evidence of efficacy for acute migraine.
Mechanism of Action
NSAIDs inhibit prostaglandin synthesis. NSAIDs reversibly inhibit cyclooxygenase (COX) 1 and 2. The NSAIDs that inhibit prostaglandin E2 synthesis are effective in treating acute migraine attacks. Aspirin acts as an irreversible COX I and 2 inhibitor.
Although not entirely understood, the current thought is that acetaminophen affects central processes, such as positive effects on the serotonergic descending inhibitory pathways. It also may affect opioidergic systems, eicosanoid systems, and the nitric oxide-containing pathways.
Administration
-
Aspirin: Peroral (PO) tablet with standard dosages of 325 mg, 500 mg, and 400 mg effervescent; treatment dosage of up to 1000 mg
-
Naproxen: PO tablet with standard dosages of 220 mg, 275 mg, 500 mg, and 550 mg; treatment dosage of 550 to 1100 mg per day in divided dosages
-
Ibuprofen: PO tablet with standard dosages of 200 mg, 400 mg, 600 mg, and 800 mg; treatment dosage of 200 to 800 mg
-
Tolfenamic acid: PO tablet with standard and treatment dosage of 200 mg
-
Diclofenac: PO tablet with standard dosages of 50 mg; treatment dosage of 50 to 100 mg
-
Piroxicam: PO capsules with standard dosages of 10 mg, 20 mg; treatment dosage of 40 mg
-
Ketorolac: Parenteral dosing with standard dosages of 30 to 60 mg; treatment dose of 30 to 60 mg
Adverse Effects
The most common adverse effects of NSAIDs are GI symptoms, which include dyspepsia, abdominal burning or discomfort, and diarrhea. Other less common symptoms include easy bruising, pruritus, rash, hypersensitivity response in asthmatics, gastritis, esophagitis, GI bleeding, renal failure, hepatic impairment, and cardiovascular events.
Besides allergic reactions, no serious side effects have been observed with acetaminophen when taken in appropriate dosages. After higher doses or prolonged duration of taking acetaminophen, hepatotoxicity, and nephrotoxicity (less common) can occur.
Contraindications
In addition to NSAID hypersensitivity reaction, another agreed-upon absolute contraindication is for those in the preoperative period of coronary artery bypass graft surgery. Warnings include those with significant cardiovascular disease, renal insufficiency, gastrointestinal erosive disorders, bleeding diathesis, and those taking warfarin.
For acetaminophen, contraindications include hypersensitivity reactions and severe active liver disease.
2.Triptans
Seven triptans have approval from the FDA and marketed for acute treatment of migraines They include sumatriptan, eletriptan, naratriptan, zolmitriptan, rizatriptan, frovatriptan, and almotriptan. Triptans are significantly more expensive than NSAIDs as a class. They are often therapeutic choices if other therapies have failed (i.e., NSAID, acetaminophen) or if the headache is severe.
Mechanism of Action
Triptans are serotonin-receptor agonists with a high affinity for 5-HT1B and 5-HT1D receptors, and variable affinity for 5-HT1F receptors. The proposed mechanism of action involves binding postsynaptic 5-HT1B receptors on the smooth muscle cells of blood vessels and presynaptic 5-HT1D receptors on the trigeminal nerve terminals and dorsal horn neurons.
Administration
Sumatriptan: PO tablet with standard dosages of 100, 50, and 25 mg; also available parenteral (though IV contraindicated because of its potential to cause vasospasm)
Eletriptan: PO tablet with standard dosages of 40 and 20 mg; contraindicated in patients with renal failure, arrhythmias, and heart failure
Naratriptan: PO tablet with standard dosages of 2.5 and 1 mg; has a sulfa group
Zolmitriptan: PO tablet with standard dosages of 5 and 2.5 mg; also available as wafer and nasal spray; wafer contains phenylalanine
Rizatriptan: PO tablet with standard dosages of 10 and 5 mg; also available as a wafer; wafer contains phenylalanine
Frovatriptan: PO tablet with a standard dose of 2.5 mg
Almotriptan: PO tablet with standard dosages of 12.5 and 6.25 mg; has a sulfa group
Adverse Effects
The most common adverse effects of triptans include pressure or tightness sensations of the chest, throat, or jaw; limb heaviness; myalgias; and fatigue. Less common adverse effects include flushing, paresthesias, dizziness, asthenia, and mental cloudiness.
Contraindications
Triptans have associations with increased blood pressure, and providers should avoid giving them to patients with uncontrolled hypertension, ischemic cardiac syndrome, cerebrovascular syndrome, or peripheral vascular condition. Patients should also not take them within 24 hours of administration, another triptan, or ergot-type medication. Triptans are also contraindicated in hemiplegic or basilar migraine and patients with hepatic impairment.
3.Antiemetics
When a migraine is associated with nausea/vomiting, an antiemetic is an excellent choice for treatment. The administration of an antiemetic is often in combination with either an NSAID or triptan, but can be used as monotherapy. Two common antiemetics used include metoclopramide and prochlorperazine. Metoclopramide has the greatest evidence for efficacy in migraine and is associated with a less likelihood of extrapyramidal side effects than prochlorperazine, but both are good initial options. Domperidone, promethazine, chlorpromazine are other examples of antiemetics.
Mechanism of Action
Metoclopramide is a benzamide that antagonizes the D2 receptor at lower doses and 5HT-3 at higher doses.
Prochlorperazine and chlorpromazine are dopamine antagonists (D2 receptor), providing antiemetic and migraine relief effects.
Administration
Metoclopramide: PO and parenteral formulations available; treatment dosages of 10 – 20 mg
Prochlorperazine: PO, parenteral and rectal formulations available; treatment dosage of 10 mg (PO and parenteral) and 25 mg (rectal)
Chlorpromazine: PO and parenteral formulations available; treatment dosage of 0.1 mg/kg up to 25 mg
Adverse Effects
Most antiemetics used for migraines are associated with a risk of QT interval prolongation and torsades de pointes. Metoclopramide, prochlorperazine, and chlorpromazine can cause dystonia, tardive dyskinesia, and akathisia (collectively known as extrapyramidal symptoms). Coadministration with diphenhydramine can prevent these symptoms. Other side effects are uncommon and can include headaches and allergic reactions such as anaphylaxis.
Contraindications
Considering the dopamine antagonists, contraindications include known hypersensitivity reactions and know extrapyramidal symptom reactions.
4.Ergotamines
Triptans have largely replaced ergotamines, as studies have shown more efficacy for triptans. Dihydroergotamine has demonstrated some efficacy, while the effectiveness of ergotamine is uncertain. In one systematic review, dihydroergotamine was not as effective as triptans, but when combined with an antiemetic, was found to be as effective as ketorolac, opiates, or valproate. Dihydroergotamine may be a useful option when patients do not respond to other medications, including triptans.
Mechanism of Action
Ergotamines, like triptans, are potent 5-HT 1b/1d receptor agonists. They involve constricting the theorized pain-producing intracranial extracerebral blood vessels at the 5-HT1B receptors and inhibit the trigeminal neurotransmission at both peripheral and central 5-HT1D receptors. They also interact with other serotonin, adrenergic, and dopamine receptors. They cause constriction of peripheral and cranial blood vessels.
Administration
Dihydroergotamine: Parenteral dosing with dosages between 0.5 – 1 mg; intranasal formulation available (4 mg)
Adverse Effects
The most common side effects include nausea and vomiting. Administer with an antiemetic. Dysphoria is another observed side effect (central 5-HT1A agonism).
Contraindications
Similar to triptans, those with cardiovascular disease should avoid the use of ergotamines. The peripheral vascular constrictive effects of ergotamines are more pronounced than triptans since triptans do not have activity at adrenergic and 5-HT2A receptors.
2)Preventive Treatments
1.Beta-Blockers
Propranolol, timolol, bisoprolol, metoprolol, atenolol, and nadolol have shown positive outcomes in migraine prevention studies. Beta-blockers with intrinsic sympathomimetic activity (such as acebutolol, alprenolol, oxprenolol, and pindolol) are not effective for migraine prevention.
Administration
Propranolol: PO immediate-release and long-acting formulations available; dose for immediate release ranging from 80 to 240 mg/day divided every 6 to 8 hours; dose for long-acting release is 80 to 240 mg/day
Timolol: PO formulation with doses of 20-30 mg/day
Bisoprolol: PO formulation with doses of 2.5 to 10 mg/day
Metoprolol: PO formulation with doses of 50 to 200 mg/day twice daily
Atenolol: PO formulation with doses of 50 to 200 mg/day
Nadolol: PO formulation with doses of 40 to 240 mg/day
Mechanism of Action
The mechanisms of action of beta-blockers in migraine prevention are not entirely understood. The thinking is that the beta-1 mediated effects could inhibit noradrenaline release and tyrosine hydroxylase activity, accounting for prophylactic action. Other possibilities include serotonergic blockade, inhibiting thalamic activity, and nitrous oxide blockade.
Adverse Effects
Common adverse effects include drowsiness, fatigue, dizziness, and weakness. Other adverse effects include weight gain, symptomatic hypotension, nausea/vomiting, diarrhea, feelings of coldness in extremities, and dry skin/mouth/eyes, bradycardia, bronchospasm, dyspnea, alopecia, visual disturbances, insomnia, sexual dysfunction, and metabolism alterations.
Contraindications
Asthma and chronic obstructive pulmonary disease have been classic contraindications because of the potential for beta-blockers to cause bronchospasm. Cocaine intoxication is another contraindication because of the risk of coronary vasospasm. This contraindication is subject to debate.
2.Antiepileptics
Several antiepileptic drugs (AEDs) have been studied and proven effective for migraine prevention, with topiramate and valproate having the best evidence.[10]
Administration
Topiramate: PO formulation with doses of 25-200 mg/day
Valproate: PO formulation of extended (once daily) and delayed (2 divided doses daily) releases are available; doses of 500-1500 mg/day
Mechanism of Action
Similar to the beta-blockers, it is unclear what effect antiepileptics have on migraine prevention. For topiramate, it blocks multiple channels such as voltage-dependent sodium and calcium channels. It also has been shown to inhibit glutamate-mediated excitatory neurotransmission, facilitate GABA-A-mediated inhibition, inhibit carbonic anhydrase activity, and reduce CGRP secretion from trigeminal neurons. For valproate, similar to topiramate, multiple mechanisms may contribute to migraine prevention. They include enhancing GABAergic inhibition, blocking excitatory ion channels, and downregulating the expression of CGRP in brain tissue.
Adverse Effects
Common adverse effects of topiramate include nausea/vomiting, diarrhea, somnolence, dizziness, weight loss, paresthesias, fatigue, nasopharyngitis, and weight loss. Other adverse effects include tachypnea, palpitations, bleeding, mood changes, dysuria, hematuria, and increased frequency of urination.
Common adverse effects of valproate include nausea/vomiting, diarrhea, abdominal pain, headache, drowsiness, hair loss, tremors, dizziness, visual disturbances, tinnitus, changes in appetite, and weight gain. Other adverse effects include confusion, severe drowsiness, bleeding, and inflammation.
Contraindications
Hypersensitivity to topiramate is a contraindication to the drug.
Contraindications to valproate usage include hepatic dysfunction, mitochondrial disorders, hypersensitivity, urea cycle disorders, and pregnancy.
3.Calcium Channel Blockers
Flunarizine is the best studied of the calcium channel blockers for migraine prevention (however not available in the U.S.). Verapamil and cinnarizine are other meds that are off-label for migraine prevention. Verapamil is probably the most commonly used calcium channel blocker for migraine prevention in the U.S.
Administration
Flunarizine: PO formulation of 5 to 10 mg/day
Verapamil: PO formulation of 120 to 480 mg/day in 3 divided doses
Mechanism of Action
Similar to the other migraine preventive treatments, the role of calcium channel blockers in migraine prevention is unclear. Flunarizine is a nonselective calcium antagonist. In addition to calcium channel activity, it blocks voltage-gated sodium channels, acts as a D2 dopamine antagonist, and increases leptin levels.
Adverse Effects
Adverse effects include constipation, cardiac conduction defects at higher doses, dizziness, constipation, headache, nausea/vomiting, flushing, edema, drowsiness, and hypotension. Lesser common adverse effects include sexual dysfunction, gingival overgrowth, and liver dysfunction.
Contraindications
Contraindications include hypersensitivity reactions, acute coronary syndrome, hypertrophic obstructive cardiomyopathy, severe stenotic heart valve defects, and cardiac conduction disorders.
4.Antidepressants
The most studied antidepressants that have shown efficacy for migraine prevention are the tricyclic antidepressant (TCA) amitriptyline and the selective serotonin reuptake inhibitor (SSRI) fluoxetine. Other TCAs and the serotonin-norepinephrine reuptake inhibitor venlafaxine have been studied and may be effective for migraine prevention, though the evidence is short.
Administration
Amitriptyline: PO formulation of 10 to 150 mg/day
Fluoxetine: PO formulation of 20 to 40 mg/day
Mechanism of Action
Similar to other migraine prevention medications, the role of antidepressants in migraine prevention is unclear. Amitriptyline is a mixed serotonin-norepinephrine reuptake inhibitor and has the following mechanisms: alpha2-adrenoceptor agonist, sodium channel blockade contributing to antimuscarinic and antihistamine effects, and cortical spreading depression.
Fluoxetine is a selective serotonin reuptake inhibitor leading to increased levels of serotonin. Noradrenaline reuptake inhibition occurs at higher doses.
Adverse Effects
Adverse effects of tricyclic antidepressants include antimuscarinic effects such as dry mouth, blurry vision, constipation, urinary retention, increased body temperature, and excessive sweating. Other side effects include morning sedation, tachycardia, vivid dreams, weight gain, hypotension, sexual dysfunction, confusion, and QT prolongation.
Adverse effects of selective serotonin reuptake inhibitors include sexual dysfunction, drowsiness, weight gain, insomnia, dizziness, headache, dry mouth, blurry vision, nausea, rash, tremors, and constipation. SSRIs can also prolong the QT interval.
Contraindications
For TCAs, coadministration with monoamine oxidase inhibitors (MAOI) is contraindicated due to the increased risk of serotonin syndrome. Hypersensitivity reactions and coadministration of cisapride are also contraindicated.
For SSRIs, coadministration of medications that significantly increase the risk of serotonin syndrome is contraindicated. These medications include monoamine oxidase inhibitors, linezolid, and methylene blue. Other contraindications include hypersensitivity reactions and coadministration with pimozide or thioridazine.
3) Other and Future Considerations
1.Triptans with NSAIDs
Research has shown the combined use of a triptan and an NSAID to be more effective than using either drug class alone for acute migraine treatment. The best-studied combination is sumatriptan plus naproxen PO. The two classes of drugs having different mechanisms of action are thought to provide better relief. Multiple studies have used sumatriptan 85 mg plus naproxen 500 mg and sumatriptan 50 mg plus naproxen 500 mg. In a meta-analysis review article, no significant difference was found between using the sumatriptan 85 mg – naproxen combo and the sumatriptan 50 mg – naproxen combo.
2.Lasmiditan
Lasmiditan is a serotonin 5-HT1F receptor agonist that has been shown effective for acute migraine treatment. The utility of this medication is that it lacks vasoconstrictor effects such as those seen in triptans, and thus offers those with cardiovascular disease an alternative to triptans. Studies have used up to lasmiditan 200 mg PO with good effect; however, there were frequent reports of adverse effects. In a recent phase, three multicenter, double-blind, randomized controlled studies, between 25.4% to 39.0% of patients receiving lasmiditan reported adverse effects. The most common adverse effects were dizziness, somnolence, and paresthesias.
3.Calcitonin Gene-Related Peptide (CGRP)
CGRP monoclonal antibodies (mAbs) are the only class of currently used preventives explicitly developed for the treatment of migraines. The current thinking is that CGRP mediates the vasodilatory component of neurogenic inflammation, as CGRP is a widely distributed vasodilator. The CGRP mAbs target either the CGRP molecule itself or the CGRP receptor. In network meta-analysis, the CGRP mAbs seemed to be as effective as other preventive treatments, but have fewer side effects. Long-term data on safety, however, is limited. These medications include erenumab, fremanezumab, and galcanezumab.
Complementary and alternative treatments
Some people get relief with therapies they use in addition to or instead of traditional medical treatment. These are called complementary or alternative treatments. For migraine, they include:
- Biofeedback. This helps you take note of stressful situations that could trigger symptoms. If the headache begins slowly, biofeedback can stop the attack before it becomes full-blown.
- Cognitive behavioral therapy (CBT). A specialist can teach you how actions and thoughts affect how you sense pain.
- Supplements. Research has found that some vitamins, minerals, and herbs can prevent or treat migraines. These include riboflavin, coenzyme Q10, and melatonin. Butterbur may head off migraines, but it can also affect your liver enzymes.
- Body work. Physical treatments like chiropractic, massage, acupressure, acupuncture, and craniosacral therapy might ease headache symptoms.
Talk to your doctor before trying any complementary or alternative treatments.
How are migraines treated?
Migraine headaches are chronic. They can’t be cured, but they can be managed and possibly improved. There are two main treatment approaches that use medications: abortive and preventive.
- Abortive medications are most effective when you use them at the first sign of a migraine. Take them while the pain is mild. By possibly stopping the headache process, abortive medications help stop or decrease your migraine symptoms, including pain, nausea, light sensitivity, etc. Some abortive medications work by constricting your blood vessels, bringing them back to normal and relieving the throbbing pain.
- Preventive (prophylactic) medications may be prescribed when your headaches are severe, occur more than four times a month and are significantly interfering with your normal activities. Preventive medications reduce the frequency and severity of the headaches. Medications are generally taken on a regular, daily basis to help prevent migraines.
What medications are used to relieve migraine pain?
Over-the-counter medications are effective for some people with mild to moderate migraines. The main ingredients in pain relieving medications are ibuprofen, aspirin, acetaminophen, naproxen and caffeine.
Three over-the-counter products approved by the Food and Drug Administration for migraine headaches are:
- Excedrin® Migraine.
- Advil® Migraine.
- Motrin® Migraine Pain.
Be cautious when taking over-the-counter pain relieving medications. Sometimes overusing them can cause analgesic-rebound headaches or a dependency problem. If you’re taking any over-the-counter pain medications more than two to three times a week, report that to your healthcare provider. They may suggest prescription medications that may be more effective.
Prescription drugs for migraine headaches include:
Triptan class of drugs (these are abortives):
- Sumatriptan.
- Zolmitriptan.
- Naratriptan.
Calcium channel blockers:
- Verapamil.
Calcitonin gene-related (CGRP) monoclonal antibodies:
- Erenumab.
- Fremanezumab.
- Galcanezumab.
- Eptinezumab.
Beta blockers:
- Atenolol.
- Propranolol.
- Nadolol.
Antidepressants:
- Amitriptyline.
- Nortriptyline.
- Zanaflex
- Doxepin.
- Venlafaxine.
- Duloxetine.
- Flexeril
- Robaxin
Antiseizure drugs:
- Valproic acid.
- Topiramate.
- Gabapentin (Neurontin )
Other:
- Steroids.
- Phenothiazines.
- Corticosteroids.
Your healthcare provider might recommend vitamins, minerals, or herbs, including:
- Riboflavin (vitamin B2).
- Magnesium.
- Feverfew.
- Butterbur.
- Co-enzyme Q10.
Drugs to relieve migraine pain come in a variety of formulations including pills, tablets, injections, suppositories and nasal sprays. You and your healthcare provider will discuss the specific medication, combination of medications and formulations to best meet your unique headache pain.
Drugs to relieve nausea are also prescribed, if needed.
All medications should be used under the direction of a headache specialist or healthcare provider familiar with migraine therapy. As with any medication, it’s important to carefully follow the label instructions and your healthcare provider’s advice.
Alternative migraine management methods, also known as home remedies, include:
- Resting in a dark, quiet, cool room.
- Applying a cold compress or washcloth to your forehead or behind your neck. (Some people prefer heat.)
- Massaging your scalp.
- Yoga.
- Applying pressure to your temples in a circular motion.
- Keeping yourself in a calm state. Meditating.
- Biofeedback.
