Postherpetic neuralgia is a painful condition that affects the nerve fibers and skin. It is a complication of shingles, and shingles is a complication of chicken pox.
If the pain caused by shingles continues after the bout of shingles is over, it is known as post-herpetic neuralgia (PHN). It is estimated that about 1 in 5 patients with shingles will go on to have PHN.
Neuralgia is neuropathic pain that occurs along the course of a nerve. It tends to happen when an irritation or damage to a nerve alters its neurological structure or function.
The sensation may be of intense burning or stabbing, and it may feel as if it is shooting along the course of the affected nerve.
Neuropathic pain comes from inside the nervous system. It is not caused by an outside stimulus, such as an injury. People often refer to it as a pinched nerve, or trapped nerve. The nerve itself sends pain messages because it is either faulty or irritated.
Symptoms of Postherpetic Neuralgia
![[neuralgia]](https://usahealthstore.com/wp-content/uploads/2021/10/neuralgia.jpg)
Symptoms are usually limited to the area of skin where the shingles outbreak first occurred and may include:
- occasional sharp burning, shooting, jabbing pain
- constant burning, throbbing, or aching pain
- extreme sensitivity to touch
- extreme sensitivity to temperature change
- itching
- numbness
- headaches
In rare cases, if the nerve also controls muscle movement, there may be muscle weakness or paralysis.
Drug Treatments for Postherpetic Neuralgia
![[PHN can follow shingles]](https://usahealthstore.com/wp-content/uploads/2021/10/phn-can-follow-shingles.jpg)
Painkillers: These may include tramadol (Ultram) or oxycodone (OxyContin). There is a small risk of dependency.
Anticonvulsants: The pain of PHN can be lessened with anticonvulsants, because they are effective at calming nerve impulses and stabilizing abnormal electrical activity in the nervous system caused by injured nerves. Gabapentin, or Neurontin, and pregabalin, also known as Lyrica, are commonly prescribed to treat this type of pain.
Steroids: A corticosteroid medication can be injected into the area around the spinal cord. Steroids should not be used until the shingles pustular skin rash has completely disappeared.
Lidocaine skin patches: Lidocaine is a common local anesthetic and antiarrhythmic drug. Applied to the skin, it can relieve itching, burning, and pain from inflammation. The patches can be cut to fit the affected area.
Antidepressants: These affect key brain chemicals, such as serotonin and norepinephrine, which influence how the body interprets pain. Examples of drugs that inhibit the reuptake of serotonin or norepinephrine are tricyclic antidepressants, such as amitriptyline, desipramine (Norpramin), nortriptyline (Pamelor), and duloxetine (Cymbalta).
Gabapentin for neuropathic pain has been found to be very effective when used correctly. Neuropathic pain refers to nerve pain and can be highly debilitating and affect the sufferer’s quality of life significantly. It occurs most commonly in patients with diabetes and after a herpes infection such as shingles. Gabapentin for neuropathic pain is available in most countries by prescription only and may be known by different trade names in different countries, according to manufacturer.
Neuropathic pain, often referred to as postherpetic neuralgia when occurring after a herpes zoster (shingles) infection, occurs due to damage caused to the nerves during the infection. This may result in various symptoms including burning pain, sensitivity to light touch or clothes, itching or numbness and may last for months to years. Treatment is often difficult and may include the use of analgesics, tricyclic antidepressants and antiepileptic drugs, like gabapentin.
Gabapentin is most commonly used to treat some types of epilepsy. It is not fully understood how gabapentin for neuropathic pain works but many studies have shown it to be effective for this indication. Due to the difficulty often experienced in trying to control neuropathic pain, the treating doctor may try different medications from different classes until pain control is achieved. In some cases this may entail the use of numerous medications together.
Treatment for Postherpetic neuralgia
Postherpetic neuralgia is a nerve disease occurs after an attack of herpes zoster infection. Herpes zoster or ‘shingles’ is a viral infection which affects the skin, especially sides of the chest, caused by varicella zoster virus. This is the same virus which causes chicken pox in children.
After an episode of herpes, the virus remains dormant in the nerve tissues of the body. This virus may become active when the immunity of the individual reduces or during convalescence after a major illness, resulting in blisters on the skin, known as shingles. It is accompanied with a rash which disappears without major consequences in about two to four weeks. Around 50% of individuals with shingles go on to develop post herpetic neuralgia (PHN) or after-shingles pain.
The neuralgia begins when the herpetic eruptions begin to heal. The pain appears usually in the affected dermatone or the affected nerve course and results in severe pain in the region which has the same nerve supply. The pain is a drawing, pricking type of intense pain, sometimes accompanied with burning sensation of the skin. The pain lasts from a few weeks to few months, rarely years.
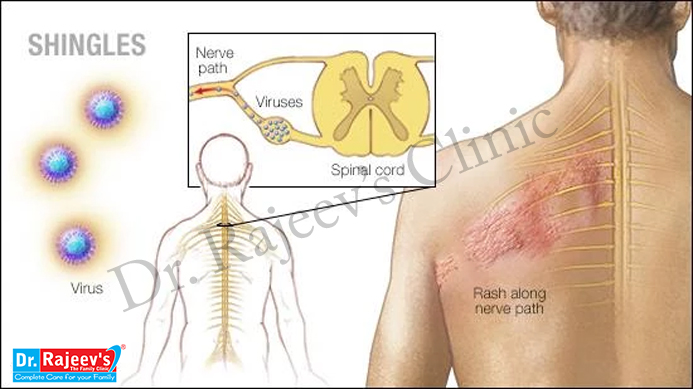
Causes
-
-
- Severe rash within three days of shingles infection
- A study shows that, 65% of patients were women
- The chances of developing PHN, increases when the shingles occurs in persons over 50 years.
- The incidence of herpes zoster is up to 15 times higher in HIV-infected patients than in uninfected persons, and as many as 25 percent of patients with Hodgkin’s lymphoma develop herpes zoster.
- Blacks are one fourth as likely as whites to develop this condition.
- Site of HZ involvement
- Lower risk – Jaw, neck, sacral, and lumbar
- Moderate risk – Thoracic
- Highest risk – Trigeminal (especially ophthalmic division), brachial plexus.
-
Signs and symptoms:
-
- A pain that continues for 3 months or more, after the healing of shingles, is defined as PHN.
- PHN pain may be burning, aching, itching and sharp and the pain can be constant or it can come and go
- The skin which was affected with blisters, may show scarring
- The involved dermatome may show altered sensations, either hypersensitivity or reduced sensitivity.
- In rare cases, where if the nerves involved also control muscle movement, the patient might also experience muscle weakness, tremor or paralysis
Postherpetic Neuralgia Treatment:
The conventional treatment is directed at pain control while waiting for the condition to resolve. Pain therapy may include multiple interventions, such as topical medications, over-the-counter analgesics, tricyclic antidepressants, anticonvulsants and a number of non medical modalities. Occasionally, narcotics may be required.
When it comes to treating postherpetic neuralgia, you may need to take a combination of medications to effectively manage your pain and other PHN symptoms. No single treatment plan is right for everyone—what medications you take will depend on your PHN symptoms.
While symptoms differ from person to person, for most people, PHN does improve over time. Researchers found that more than half of all patients with PHN stop experiencing pain within one year.1
Fortunately, during that period of intense pain and other symptoms, there are certain medications that you can take to significantly help control postherpetic neuralgia symptoms.
Before trying a prescription medication, your doctor will most likely want you to try an over-the counter (OTC) analgesic (painkiller) medication, such as acetaminophen or non-steroidal anti-inflammatory drugs (NSAIDs). These medications can help relieve pain and other PHN symptoms.
Tylenol is an example of acetaminophen, and Advil is an example of an NSAID you can take to help treat PHN.
Another OTC medication you may want to try for PHN is capsaicin cream. This cream—made from hot chili pepper seeds—is applied to the affected skin, and it can be helpful for reducing PHN-related pain. But this cream can be painful, so talk to your doctor about how much you should apply.
If these medications aren’t strong enough to treat your PHN symptoms, your doctor may suggest some of the prescription medications below to treat your postherpetic neuralgia.
-
- Tricyclic antidepressants, such as amitriptyline (Elavil), nortriptyline (Pamelor), and desipramine (Norpramin) are effective at treating postherpetic neuralgia pain. Other classes of antidepressant are also helpful. All classes of antidepressant take a few weeks to start working.
- Anticonvulsants, developed to control seizures, can help reduce the pain of PHN. These include gabapentin (Neurontin), carbamazepine (Tegretol) and pregabalin (Lyrica). Gabapentin enacarbil (Horizant) and gabapentin (Gralise) are approved by the FDA for the treatment of PHN in adults.
- Anti-viral drugs valacyclovir and acyclovir are also becoming medications of choice for treating postherpetic neuralgia.
- Lidocaine Patches for Postherpetic Neuralgia. Lidocaine patches are FDA-approved to treat PHN. The medication in the patch—lidocaine—can penetrate your skin and go to the nerves that are sending the pain signals. A benefit of lidocaine patches is that they don’t numb the skin.
- Prescription capsaicin patches. These patches contain a very high concentration of the chili pepper extract capsaicin. The capsaicin patch Qutenza is applied in a doctor’s office for one hour every three months.
If you have severe pain and other medications don’t work for you, your doctor may want you to try an opioid. Tramadol (eg, Ultram) is an example of a relatively weak opioid that can be used to help you manage PHN. Your doctor may have you try a weaker opioid first. Opioids, such as morphine (MS Contin), oxycodone (OxyContin), and hydrocodone (Vidocin), are also used to treat moderate to severe pain of postherpetic neuralgia.
Homoeopathic Medicine:
Mezereum – For Postherpetic Neuralgia with Intense Burning
Mezereum is rated among the best medicines for postherpetic neuralgia. It is the best-suited prescription when postherpetic neuralgic pains are violent and attended with marked burning. Mezereum is the most helpful among medicines for postherpetic neuralgia in postherpetic pains located in the face. The pain in the face may get worse while eating.
Warmth brings relief. Mezereum is also helpful during active herpes zoster where eruptions are present. The key symptoms to look out for before prescribing Mezereum during herpes zoster infection are violently itching vesicles with shining red areola and intense burning.
2. Ranunculus Bulbosus – For Pains coming in Paroxysms
Another of the prominently indicated medicines for postherpetic neuralgia is Ranunculus Bulbosus. It is indicated for sharp, shooting, postherpetic neuralgic pains that come in paroxysms.
It is also one of the top listed medicines for intercostal neuralgia following herpetic infection. Ranunculus Bulbosus is also indicated for herpes zoster when the vesicles eruptions are bluish in colour. The eruptions are attended with itching and burning symptoms which worsen on contact.
3. Rhus Tox – One of the best Medicines for Postherpetic Neuralgia
Rhus Tox also figures on the list of highly effective medicines for postherpetic neuralgia. It is one of the best medicines for postherpetic neuralgia where the pains are attended with marked restlessness. The skin is sensitive to cold air in such cases. In herpes zoster, Rhus Tox is the most preferred among medicines when the vesicles are yellowish with itching and stinging.